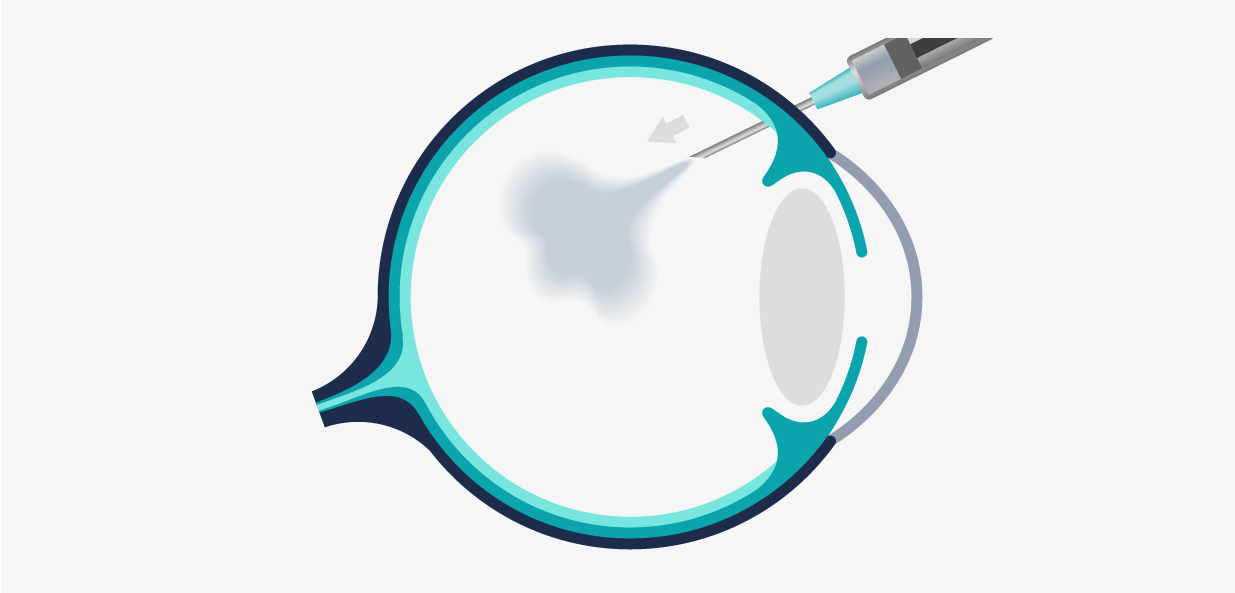
Intravitreal injections are used to administer drugs in the eye to treat eye diseases and protect vision. Through an injection, the appropriate medication is introduced into the vitreous cavity, a space located at the back of the eye, behind the lens (as seen in the image).
Injecting these medications directly into the vitreous cavity can treat certain eye diseases and protect vision. Some of the diseases that most frequently require intravitreal injections are:
Intravitreal injections are a far more effective way for drugs to reach and treat the centre of the eye than taking them orally or injecting them into a vein. Intravitreal injections allow for higher and more intense doses than would be safe to take orally.
Intravitreal injections can be used to administer antibiotics to treat endoftalmitis (inflammation of the interior of the eye); a class of drugs known as antiVEGF for conditions including wet AMD, diabetic retinopathy or vascular occlusions in the retina, or corticosteroids (steroid hormones) for intraocular inflammations such as uveitis or macular edema.
The injections are administered in an operating theatre under topical anaesthesia. Before proceeding, the eye and eyelids are disinfected, under aseptic conditions. It is a usually fast and painless procedure, and causes little discomfort in the postoperative period.
After the injection, you may experience a foreign body sensation, pressure in the eye or mild and nonspecific discomfort, although there is usually no pain. There may also be a small subconjunctival hemorrhage or you may see “floaters“. Both effects disappear over time.
It is important to avoid touching your eyes and swimming for several days.
If you experience pain or discomfort, eye reddening, sensitivity to light or reduced vision, you should see the ophthalmologist immediately.
Although the risk of complications is extremely low, the most likely complication is infection. Nevertheless, preparing the eye in sterile conditions in the operating theatre means that this is very unlikely. Other less serious possible complications are equally rare.

Contact us or request an appointment with our medical team.