

Cataract surgery is a short procedure (about 20 minutes) performed with local anesthesia.

It is an outpatient intervention: the patient can go back home the same day on their own.

The postoperative is quick and painless.
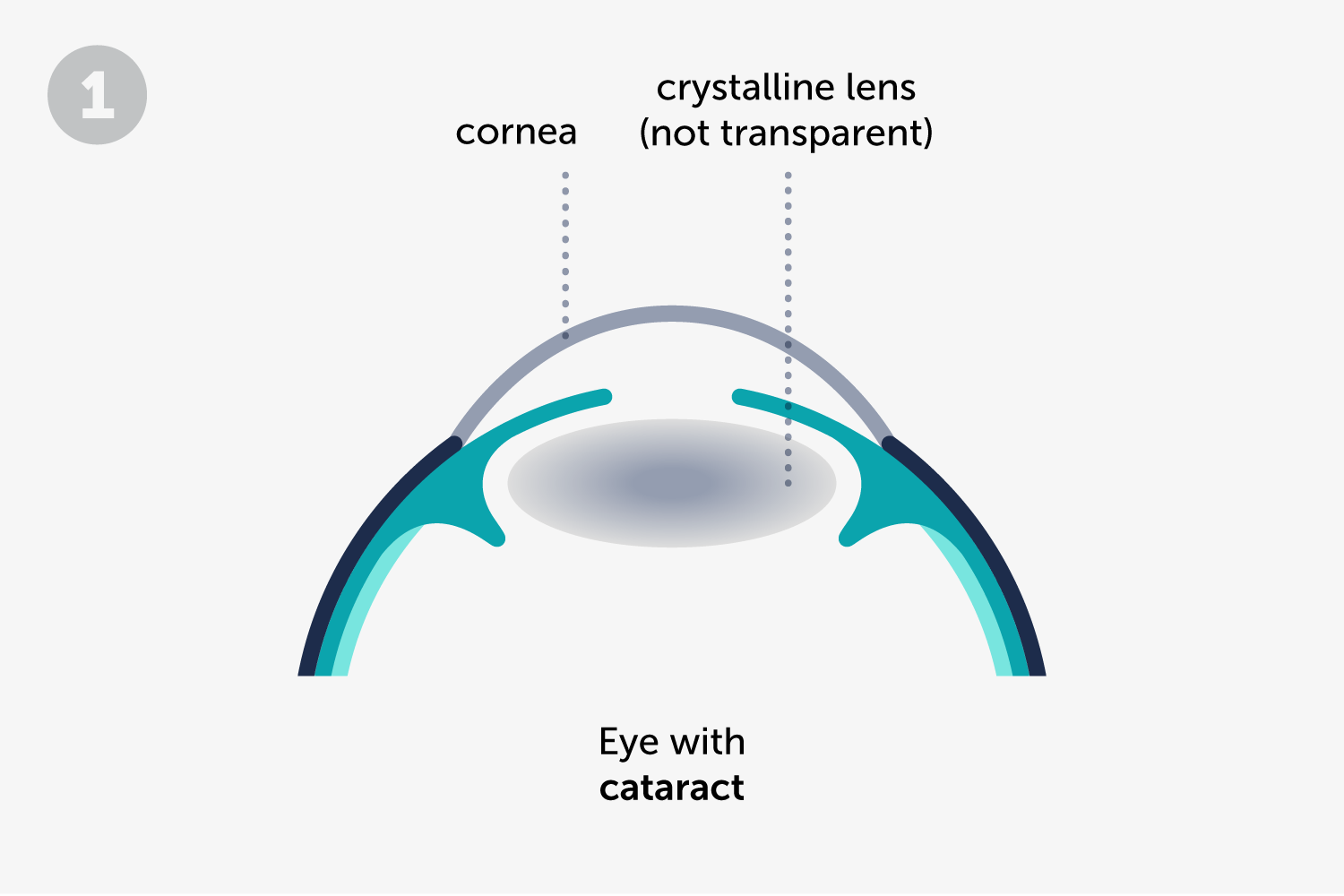
A cataract is an opacification of the crystalline lens, one of the two natural lenses in the eye; the other one is the cornea. The main symptom of cataracts is a slow, progressive vision loss, which usually develops during months or years and that can affect one or both eyes.
There are several types of cataracts (nuclear, subcapsular posterior and cortical), but the treatment in all of them is surgical, in an intervention called phacoemulsification of the crystalline lens.
Yes. During cataract surgery, we must implant an intraocular lens, which can be customized for each patient in order to both eliminate cataracts and correct refractive errors in the eye: myopia, hyperopia, presbyopia and astigmatism. Thus, after surgery, the patient regains the vision they had lost because of the cataract and could also reduce their dependence on glasses.
Depending on the used kind of intraocular lens, in some cases the patient could reduce their dependence on glasses after cataract surgery.

A team of ophthalmologists with wide experience and prestige in the study and treatment of cataracts.

We use the most advanced technology and incorporate the latest scientifically proven innovations.

ICR is an integral ophthalmology center that has all subspecialties and a 24/7 emergency service.
Trifocal lenses are the lenses of choice for patients who decide to enjoy independence from the glasses after the operation, thanks to the excellent visual results they provide at all distances. At ICR we use state-of-the-art trifocal lenses, which have a focus for distant, intermediate and near vision and, in their toric version, also allow the correction of astigmatism. The objective is that after surgery the residual graduation of the eye is as low as possible and the patient can enjoy the desired independence of the glasses.
In cases where, due to the characteristics of the eye, trifocal lenses are not the best option, there are alternatives such as the so-called extended focus lenses (also known as EDOF), that allow these patients to achieve not only good visual acuity from a distance but a very good functional vision at intermediate distance. At ICR we are pioneers in the use of this type of intraocular lens and we have implanted them with very good results.
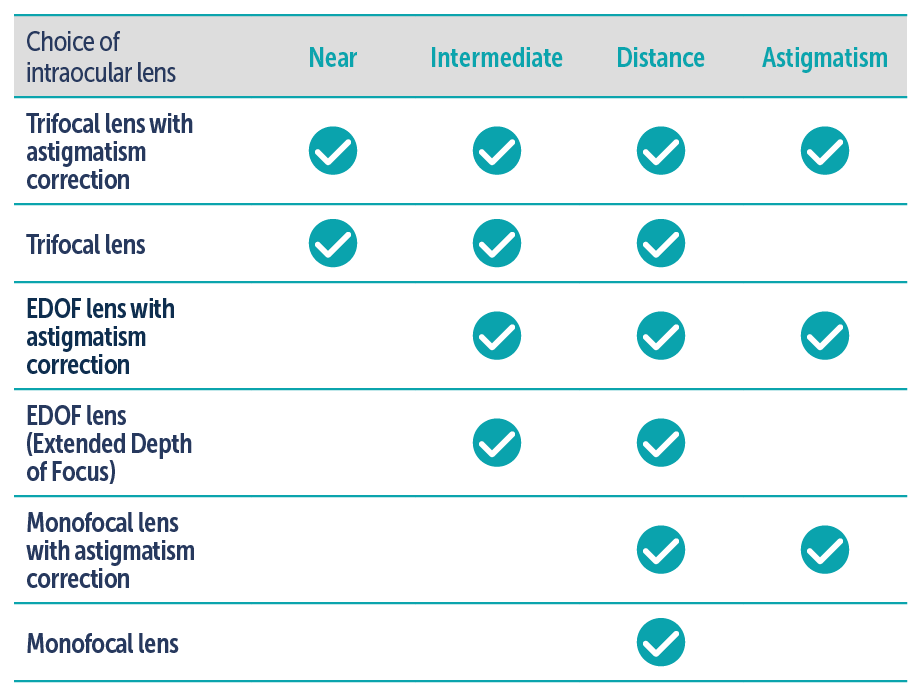
Our ophthalmologists specialising in cataracts will advise each patient the best option based on their needs, lifestyle and eye medical history.
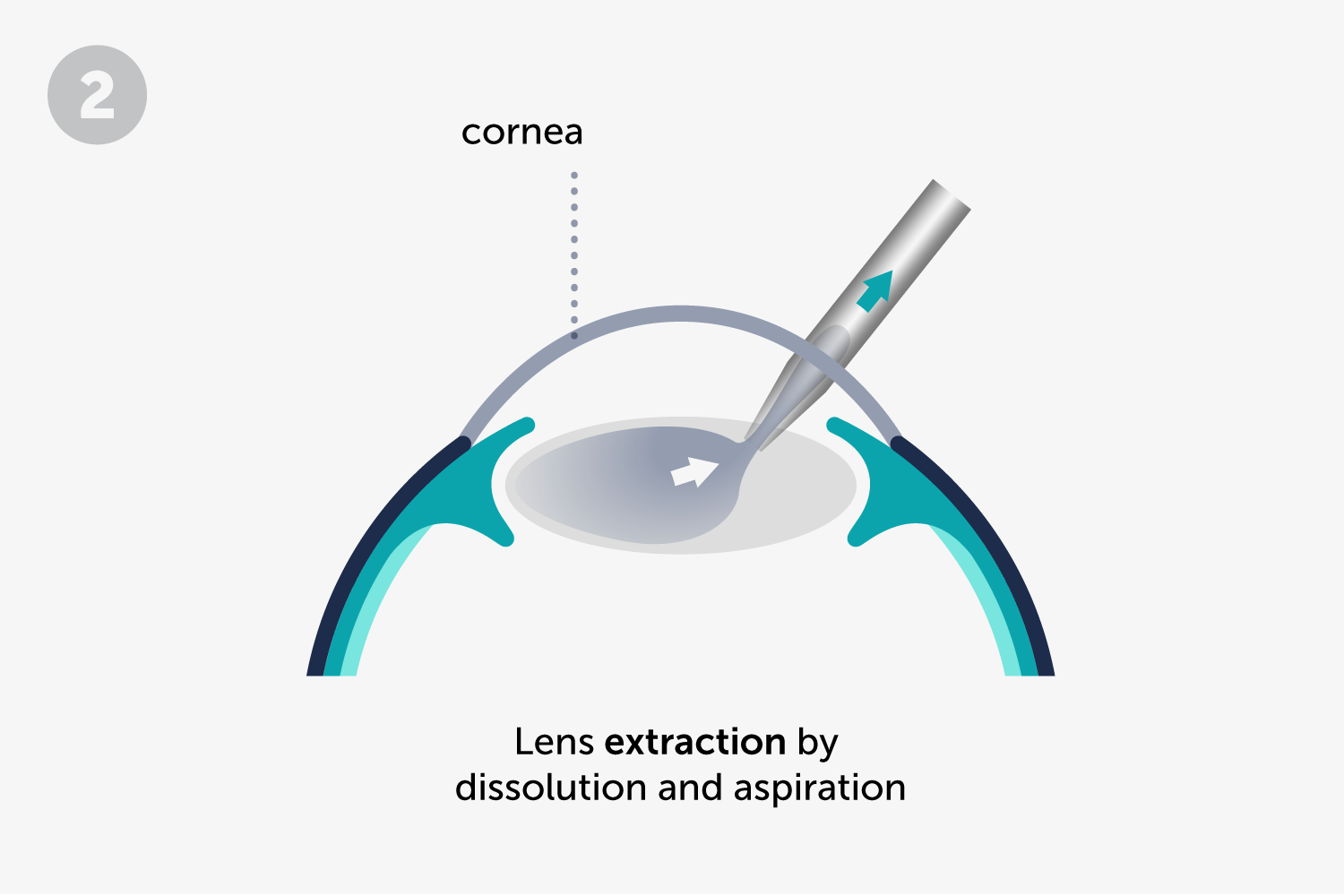
Cataract surgery is one of the most frequent at ICR. We perform it through a procedure called phacoemulsification, which uses ultrasonic energy to extract the opacified crystalline lens (cataract) and then replace it with an intraocular lens.
It is an outpatient procedure (it does not require hospitalization), that uses a microincision of only 2 mm. We use topical anesthesia (eyedrops) along with a mild sedation. The opacified natural lens is extracted by dissolution and aspiration and an intraocular lens is implanted to replace the opacified one. When the procedure is complete, the patient can go home on their own.
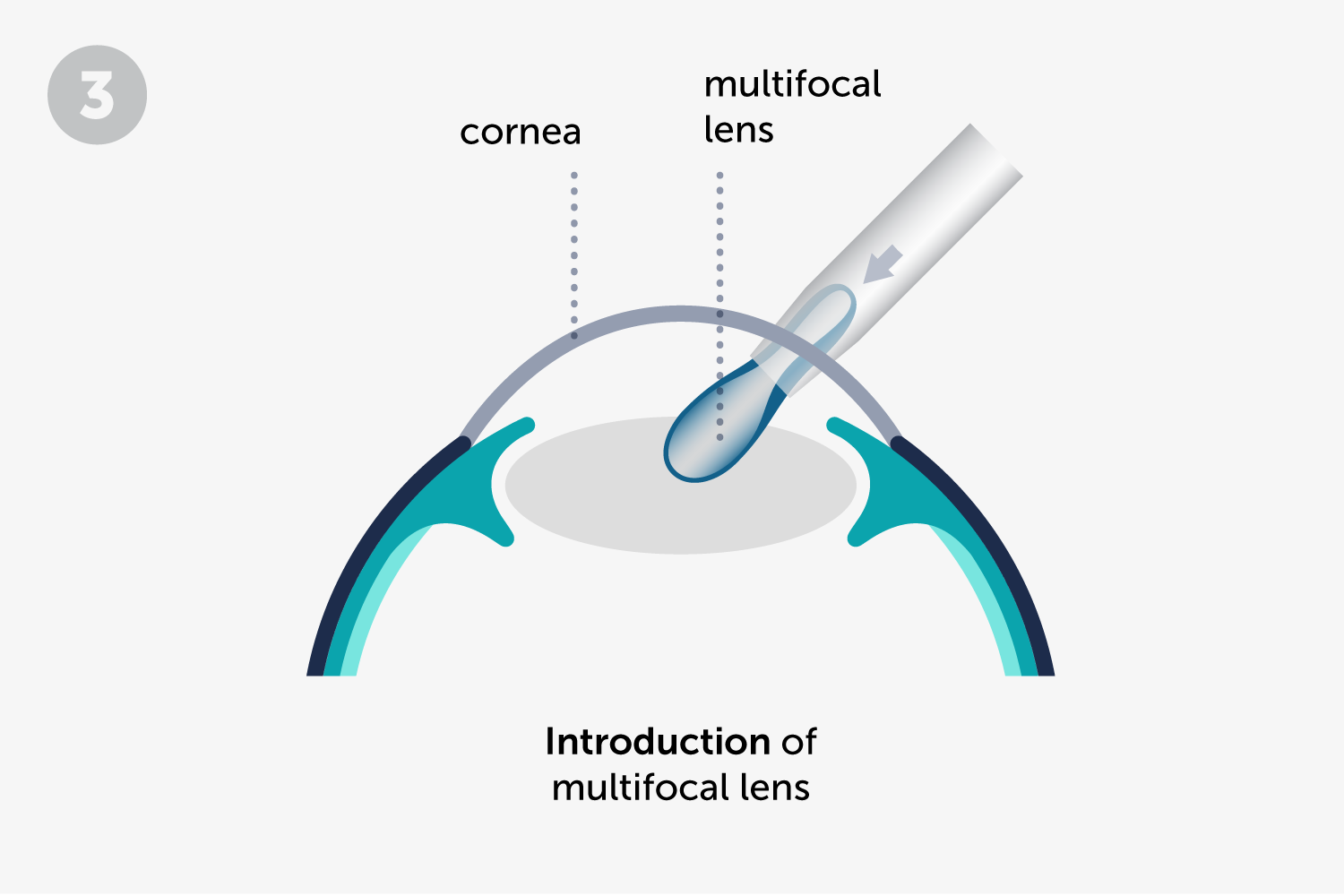
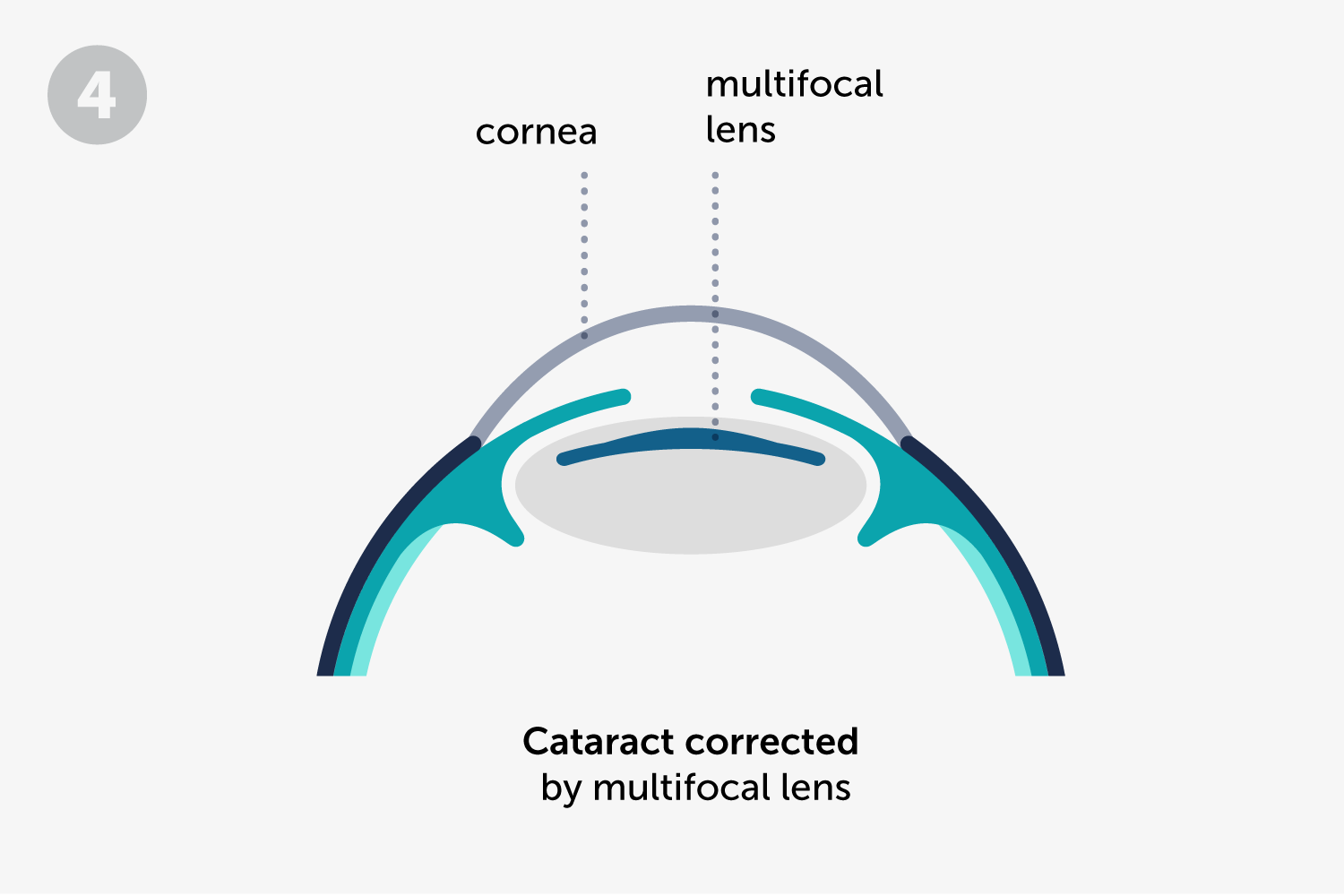
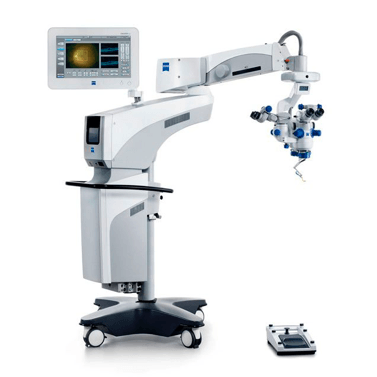
At ICR we have the most advanced surgical microscopes, which allow us to implant monofocal and premium intraocular lenses (trifocal and toric) with maximum precision.
ICR was one of the first centers in Spain to have the Cataract Suite Markerless system, the most advanced microscopy system in cataract surgery. This innovative device allows the information collected by the different teams involved in the operation to be automatically combined. It is currently the safest, most accurate and most comfortable technology.
We also have the first optical device for cataract biometry, as well as highly secure phacoemulsificators that allow the surgeon to act with higher precision, better control the intraocular pressure and ultimately performe the procedure in a more effective and safe manner.
The intraocular lens used to replace the opaque lens allows correction of the patient’s refractive problems, such as nearsightedness, farsightedness, astigmatism or presbyopia. In this way, and depending on the type of intraocular lens chosen, the patient can reduce or even eliminate his dependence on glasses.
Most age-related cataracts develop gradually, so obvious symptoms may not be apparent at first. As the cataract progresses, it can cause more noticeable symptoms, such as blurred or double vision, dim or yellowish vision, difficulty seeing at night, or sensitivity to light.
In order to diagnose a cataract, the patient must go to a specialist, who will ask about their medical history (medicines, systemic diseases, trauma, eye diseases …) and will perform a complete eye study, which will include tests such as a pupillary and refractive examination, a biomicroscopy, a tonometry and a study of the fundus among others.
The cataract operation usually takes approximately 20 minutes. This is an outpatient intervention (does not require hospital admission), for which topical anesthesia (drops) is used.
The postoperative period of a cataract surgery is usually painless and causes little discomfort, which disappears after a few days. Some of the discomforts that can be experienced are dry or gritty eyes, glare, etc.
After the intervention, the patients can go back to their normal life, taking some precautions during the first week, like avoiding physical effort or sudden movements, not rubbing their eyes, sleeping on their back or on the side of the eye that has not been operated, wearing sunglasses to go out and taking care of hygiene measures, in addition to following the treatment and controls indicated by their ophthalmologist.
Many people believe that cataracts only affect older people. However, there are also cases of cataracts in children. These cataracts can be congenital (they are present at birth) or acquired (they appear later).
Because children’s vision is in the developmental process until age 8 or 10, untreated pediatric cataracts can lead to long-term vision problems. For this reason, early detection and treatment can prevent permanent vision loss.
The treatment for childhood cataracts may vary depending on its type and severity. In some cases, they require surgical intervention in order to be removed. In others, surgery is just the first step to complete eye rehabilitation, and treatment must continue with the aim of repairing the connections between the brain and the eye and for the latter to learn to focus correctly.
The majority of cataract cases appear from the age of 50 or 60 when, due to age, the tissue that forms the lens of the eyes loses flexibility, transparency and thickness. However, beyond age, there are other eye pathologies, previous eye surgeries or diseases such as diabetes that can also cause the creation of cataracts.
Contrary to what was previously believed, it is currently recommended to perform the operation when the cataracts begin to affect the patient’s vision. In this way we avoid long waits, loss in the quality of life of the patient and complicated interventions and postoperative.
Patients who have immature or incipient cataracts and do not require surgery should go for an annual or even more regular review if there is a symptomatic decrease in vision. Ultimately, the only way to remove cataracts and restore lost vision is surgery.
Although the percentage of serious complications derived from a cataract operation is low, if they occur in both eyes after bilateral surgery, they can significantly disable the patient. Thus, good judgement suggests that is better to wait a few days (one or two weeks) between surgery on one eye and the other.
Secondary cataract is an opacification of the posterior lens capsule that can appear a few months or years after undergoing a cataract extraction operation. Up to 20 % of patients who have undergone cataract extraction may experience them.
It is not possible to know if a patient will develop a secondary cataract after a cataract extraction, but it is usually developed mainly by younger patients who have undergone cataract surgery.
The treatment that is usually recommended after the appearance of a secondary cataract is a capsulotomy, which consists of making an incision in the posterior capsule with the help of YAG Laser.
Yes, in fact, we do it regularly. In these cases, it is just important to know that the patient has undergone refractive surgery, so that the ophthalmologist can request the appropriate tests to assess the shape of the cornea. Next, and by means of a series of specific formulas, the power of the lens to be placed inside the eye during cataract surgery will be determined. In no case, therefore, does refractive surgery represent any problem or pose any added difficulty when performing cataract surgery.
In order to offer an estimate price for each patient, we kindly ask you to contact us.
The ICR Cataract Department is made up of a team of professionals with extensive experience and recognized prestige, dedicated exclusively to the study and surgical treatment of cataract problems, with extensive experience in the specialty and linked to various scientific societies. All of them regularly participate in medical congresses and meetings both nationally and internationally, as well as in research and development projects.
Experience, technology and medical treatment with a human touch.

Contact us or request an appointment with our medical team.